Case Presentation
Application of vacuum assisted closure in the treatment of surgical site deep infection spinal
Aplicación del cierre asistido por vacío en el tratamiento de la infección profunda del sitio quirúrgico espinal
Son Thach Mao1 https://orcid.org/0009-0009-5537-2577
Ngoc Hieu Nguyen2* https://orcid.org/0000-0001-6091-3491
1Trieu An Hospital. Ho Chi Minh City, Vietnam.
2University of Medicine and Pharmacy at Ho Chi Minh City. Ho Chi Minh City, Vietnam.
*Correspondence author. Email: ngochieu0707@gmail.com
ABSTRACT
Background: Treatment of spinal infections is a current challenge with a high rate of complications and death. Currently, there are many approaches to treat infections of the spine early, but there is no specific regimen.
Objective: To present two cases of deep spinal infection treated with surgery and vacuum-assisted closure combined with antibiotics as a potentially effective treatment option.
Clinical Case: Two clinical cases about infection of the deep and early spine incision caused by S. epidermidis, treated with wound irrigation and debridement, spine fusion tools, and use it at the same time combined with vacuum assisted closure.
Conclusions: Early diagnosis combined with timely surgical debridement and vacuum-assisted closure, alongside appropriate antibiotic therapy, may reduce treatment duration and promote recovery in postoperative spinal wound infections.
Keywords: Spine; Staphylococcus epidermidis; surgical wound infection; vacuum assisted closure.
RESUMEN
Antecedentes: El manejo de las infecciones de la columna vertebral es un reto clínico relevante, debido a su elevada tasa de complicaciones y mortalidad. Aunque se han descrito diversas estrategias para el tratamiento temprano de estas infecciones, todavía no existe un protocolo estandarizado que garantice resultados consistentes.
Objetivo: Presentar dos casos de infección profunda del sitio quirúrgico espinal tratados mediante intervención quirúrgica y aplicación de un sistema de cierre asistido por vacío, combinado con terapia antibiótica, como una alternativa terapéutica potencialmente eficaz.
Casos Clínicos: Dos pacientes con infección profunda y temprana de la incisión espinal causada por Staphylococcus epidermidis. Ambos fueron manejados mediante irrigación y desbridamiento quirúrgico, mantenimiento de la instrumentación vertebral y aplicación simultánea de un sistema de cierre asistido por vacío, asociado con tratamiento antibiótico dirigido.
Conclusiones: El diagnóstico precoz, combinado con el desbridamiento quirúrgico oportuno y el cierre asistido por vacío, junto con una terapia antibiótica adecuada, puede reducir la duración del tratamiento y favorecer la recuperación en las infecciones de la herida quirúrgica postoperatoria de la columna vertebral.
Palabras clave: cierre asistido por vacío; columna vertebral; infecciones del sitio quirúrgico; Staphylococcus epidermidis.
Received: 30/12/2025
Approved: 23/02/2026
INTRODUCTION
Postoperative spinal surgical site infection remains a serious and debilitating complication, contributing to increased morbidity, prolonged hospitalization, higher medical costs, and mortality, with an incidence ranging from 1% to 15%.(1)
Staphylococcus epidermidis, a Gram-positive commensal bacterium of the human skin and mucosa, can become an opportunistic pathogen commonly associated with infections related to prosthetic devices, spinal instrumentation, and other surgical procedures.(2,3,4) Early diagnosis of postoperative spinal infection is often difficult, as clinical and radiological findings may overlap with postoperative fluid collection or edema, especially in the presence of metallic implants.
Effective management requires timely wound irrigation and debridement, coupled with appropriate antibiotic therapy, to eradicate infection while preserving the fixation system whenever possible. In recent years, negative pressure wound therapy, or Vacuum-Assisted Closure (VAC), has become an important adjunctive treatment for infection control and wound healing. VAC therapy helps remove exudate, decrease bacterial load, reduce local edema, and improve perfusion, promoting granulation tissue formation and faster healing.(5) Although vacuum-assisted closure has been increasingly applied in the management of surgical site infections, recent literature specifically addressing its use in deep spinal surgical site infections remains limited. Most available evidence continues to consist of earlier case series and retrospective reports, reflecting the relative rarity of this complication and the absence of large contemporary studies.
This report describes two cases of deep postoperative spinal infection caused by S. epidermidis, successfully treated through surgical debridement, targeted antibiotic therapy, and VAC-assisted wound management.
CLINICAL CASE
Case 1
A 47-year-old man with chronic hepatitis B on antiviral therapy, presented with recurrent low back pain radiating to the right gluteal region, worsening over the past two months despite conservative management. He had undergone L4–L5 discectomy 14 years earlier.
Physical examination revealed a Schober’s test of 12/10 cm and positive bilateral Lasègue’s signs. Magnetic Resonance Imaging (MRI) revealed lumbar canal and foraminal stenosis at L3–S1 due to disc protrusion and ligamentum flavum hypertrophy.
The patient underwent posterior decompression and interbody fusion using a polyetheretherketone (PEEK) cage and titanium pedicle screw fixation. Cefoxitin (2 g) and amikacin (0.5 g) were administered prophylactically. The postoperative course was initially uneventful, and he was discharged on day four.
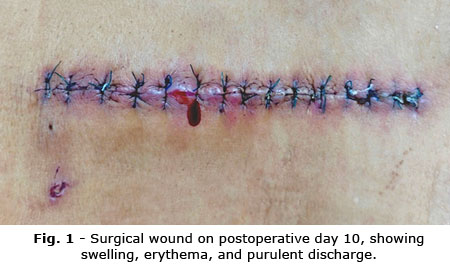
However, seven days later, wound redness, swelling, and serous discharge developed (Fig. 1). Laboratory findings showed leukocytosis and elevated C reactive protein (CRP) (2.98 mg/dL). Empirical vancomycin and amikacin were started. Pus culture yielded S. epidermidis, resistant to several β-lactams; therapy was adjusted to intravenous ciprofloxacin.
Re-exploration revealed necrotic tissue and purulent exudate around the fixation hardware. Extensive debridement and irrigation with saline and povidone-iodine were performed while retaining the stable implants. Vancomycin powder (1 g) was applied locally, and a continuous vacuum-assisted closure (VAC) system was placed at 125 mmHg (Fig. 2). Six days later, healthy granulation tissue was observed, and VAC therapy was continued intermittently. The patient received oral linezolid 600 mg twice daily for four weeks. Complete wound healing occurred within ten days after VAC removal, with no recurrence or residual infection during follow-up (Fig. 3).
Case 2
A 44-year-old man with a 4-year history of chronic low back pain experienced worsening symptoms over the past year, with radiation to both posterior thighs and legs, numbness, and gait disturbance unresponsive to medical therapy. He had long-term corticosteroid use and presented with cushingoid features.
Examination showed lumbar tenderness, Schober’s test 12/10 cm, bilateral sensory loss in the posterior thighs and legs, reduced patellar and Achilles reflexes, and ankle motor strength graded 4/5. Serum cortisol was 17.57 nmol/L. MRI demonstrated lumbar canal stenosis from L3–S1 due to disc herniation and ligamentum flavum hypertrophy.
He underwent posterior decompression, interbody fusion, and pedicle screw fixation using titanium alloy screws and PEEK cages. Prophylactic cefoxitin (2 g) and amikacin (0.5 g) were administered for four days postoperatively. The wound healed initially, and he was discharged on day 4.
Twelve days later, the patient developed fever, wound erythema, tenderness, and purulent discharge. Laboratory results showed elevated CRP (10.72 mg/dL) and low albumin (32.4 g/L). Empiric vancomycin and amikacin were started, and VAC therapy was applied at –125 mmHg. Culture revealed S. epidermidis resistant to multiple antibiotics. Amikacin was replaced with tetracycline, and surgical debridement with copious saline and povidone-iodine irrigation was performed. The implants were stable and retained. Vancomycin powder (1 g) was applied locally, and VAC therapy was continued. After 72 hours, repeat cultures were negative. Progressive wound granulation was achieved, allowing partial closure and intermittent VAC use. The patient received oral linezolid 600 mg twice daily for six weeks. Complete wound healing was obtained one week after VAC removal, with no signs of recurrence
Bioethical aspects
Written informed consent was obtained from the patients for publication of this cases report.
COMMENTS
Postoperative spinal wound infection is an uncommon but serious complication, generally classified as superficial or deep. Superficial infections involve only skin and subcutaneous tissues, whereas deep infections extend to fascial layers. In both presented cases, intraoperative findings revealed necrotic tissue and purulent discharge beneath the fascia surrounding the fixation system, consistent with deep infection. Both cultures grew S. epidermidis, showing resistance to penicillin-related antibiotics. According to Otto M,(6) S. epidermidis is a major cause of device-related infections due to its biofilm-forming ability, which protects bacteria from immune responses and antibiotics. Previous studies reported 82.6–95.65% penicillin resistance linked to the mecA gene encoding low-affinity penicillin-binding protein.(7,8)
Patients received empirical vancomycin (2 g/day) plus amikacin (1 g/day). After susceptibility testing, amikacin was replaced by ciprofloxacin (0.4 g/day) in Case 1 and tetracycline (1 g/day) in Case 2. After five days, both underwent surgical debridement, and repeated cultures were negative. Fixation devices were retained, and 1 g vancomycin powder was applied before closure. Early debridement is vital to remove necrotic tissue and prevent chronic infection. Divi SN et al.(9) reported implants can be safely retained in early infection (< 30 days) if stable. Xie ll et al.(10) found topical 0.5-2 g vancomycin with VAC therapy reduces bacterial load and accelerates healing. However, biofilms may decrease vancomycin efficacy, so antibiotic therapy must be carefully monitored.(11)
Before VAC application, debridement and irrigation were performed, and then continuous negative pressure (125 mmHg) applied to improve microcirculation, remove exudate, and promote granulation. VAC duration was 11 days in Case 1 and 19 days in Case 2, both showing rapid wound healing, consistent with ElDegwy M et al.(12) and others authors.(13,14)
Early diagnosis and timely intervention are crucial in the management of postoperative spinal wound infections. In addition to appropriate antibiotic therapy, the combination of surgical debridement and VAC therapy plays a significant role in reducing treatment duration and accelerating recovery in affected patients.
Acknowledgements
The authors would like to express their sincere gratitude to Trieu An Hospital, Vietnam, for its valuable support and for providing the necessary conditions that enabled the research team to conduct this study. The authors also wish to thank participating patient for their cooperation and for providing informed consent to take part in this research.
BIBLIOGRAPHIC REFERENCES
1. Sawires AN, Park PJ, Lenke LG. A narrative review of infection prevention techniques in adult and pediatric spinal deformity surgery [Internet]. J Spine Surg. 2021;7(3): 413–21. DOI: 10.21037/jss-21-10
2. Brown MM, Horswill AR. Staphylococcus epidermidis - skin friend or foe? [Internet]. PLoS Pathog. 2020;16(11): 1-6. DOI: 10.1371/journal.ppat.1009026
3. Bose S, Ghosh AK. A challenge to medical science [Internet]. J Clin Diagn Res. 2011 [access: 10/08/2025];5(1):127–130. Available from: https://www.jcdr.net/article_fulltext.asp?issn=0973-709x&year=2011&volume=5&issue=1&page=127&issn=0973-709x&id=1129
4. Palanichamy N, Kumar P, Mickymaray S, Alothaim AS, Somasundaram J, Rajan M. Recent Developments in Methicillin-Resistant Staphylococcus aureus (MRSA) Treatment: A Review [Internet]. Antibiotics. 2022;11(5):606. DOI: 10.3390/antibiotics11050606
5. Đạo NH, Pham TL, Đao TMT, Đao TH. Đánh giá kết quả ứng dụng liệu pháp hút áp lực âm chăm sóc khuyết hổng phần mềm tại Bệnh viện Hữu nghị Việt Tiệp Hải Phòng [Internet]. Tạp chí Khoa học Điều dưỡng. 2020 [access: 01/10/2025]; 3(4):84-9. Available from: https://jns.vn/index.php/journal/article/view/265
6. Otto M. Staphylococcus epidermidis - the ‘accidental’ pathogen [Internet]. Nat Rev Microbiol. 2009 [access: 01/10/2025];7(8):555-67. Available from: https://www.nature.com/articles/nrmicro2182
7. Chabi R, Momtaz H. Virulence factors and antibiotic resistance properties of the Staphylococcus epidermidis strains isolated from hospital infections in Ahvaz, Iran [Internet]. Trop Med Health. 2019;47:56. DOI: 10.1186/s41182-019-0180-7
8. Chambers HF, Hartman BJ, Tomasz A. Increased amounts of a novel penicillin-binding protein in a strain of methicillin-resistant Staphylococcus aureus exposed to nafcillin [Internet]. J Clin Invest. 1985;76(1):325–31. DOI: 10.1172/JCI111965
9. Divi SN, Chiba K, Oner FC, Malham GM, Rahimi-Movaghar V, Joaquim AF, et al. The management of early post-operative spinal infection in the presence of implants, interbody cages, and bone grafting [Internet]. Switzerland, Davos: AO Spine Clin Expert Advice Forums; 2017. [access: 01/10/2025]. Available from: https://int.aofoundation.org/spine/-/media/project/aocd/aospine/documents/post-operative_spinal_infection_in_the_presence_of_implants1.pdf
10. Xie Ll, Zhu J, Yang M, Yang C, Luo S, Xie Y, et al.. Effect of intra-wound vancomycin for spinal surgery: a systematic review and meta-analysis [Internet]. Orthop Surg. 2017;9(4):350–8. DOI: 10.1111/os.12356
11. Richards GK, Prentis J, Gagnon RF. Antibiotic activity against Staphylococcus epidermidis biofilms in dialysis fluids [Internet]. Advances in Peritoneal dialysis - Conference on Peritoneal Dialysis. 1989 [access: 01/10/2025];5:133-7. Available from: https://pubmed.ncbi.nlm.nih.gov/2577396/
12. ElDegwy M, Omar A, Elasheery AO, Shaaban MA. Strategic management of deep sternal wound infection using vacuum assisted closure system [Internet]. J Adv Pharm Educ Res. 2017 [access: 1/10/2025];7(4):443–449. Available from: https://www.researchgate.net/publication/324527672_Strategic_management_of_deep_sternal_wound_infection_using_Vacuum_assisted_closure_system
13. Domkowski PW, Smith ML, Gonyon DL Jr, Drye C, Wooten MK, Levin LS, et al. Evaluation of vacuum-assisted closure in the treatment of poststernotomy mediastinitis [Internet]. J Thorac Cardiovasc Surg. 2003;126(2):386–9. DOI: 10.1016/S0022-5223(03)00352-0
14. Derin AKCS, Negatif SYİ. Role of negative-pressure wound therapy in deep sternal wound infection after open heart surgery [Internet]. Artificial Organs. 2012 [access: 1/10/2025]; 36(5):A29. Available from: https://www.ovid.com/journals/artorg/abstract/00000888-201205000-00100~role-of-negative-pressure-wound-therapy-in-deep-sternal
Conflicts of interest
No benefits have been or will be received from a commercial party related directly or indirectly to the subject matter of this article.
Financial information
None.
Data availability
The data used to present this case correspond to the clinical records of a patient diagnosed and managed at Trieu An Hospital, Ho Chi Minh City, Vietnam.