Research Article
Predictive modeling of direct medical costs among frail older adults with diabetes mellitus in a rural outpatient setting
Modelación predictiva de los costos médicos directos en adultos mayores frágiles con diabetes mellitus, en un contexto ambulatorio rural
Ngoc Tuyet Nguyen1,3 https://orcid.org/0009-0001-3058-0291
Cuong Quoc Hoang2 https://orcid.org/0000-0003-1934-7138
Minh Trung Nguyen3 https://orcid.org/0009-0004-4379-7627
Van De Tran3* https://orcid.org/0000-0003-0421-5079
1Phong Dien Commune Health Station. Can Tho City, Viet Nam.
2Can Tho Department of Health. Can Tho City, Vietnam.
3Can Tho University of Medicine and Pharmacy. Can Tho City, Vietnam.
*Corresponding author. Email: tvde@ctump.edu.vn
ABSTRACT
Background: Diabetes mellitus and frailty are associated with increasing healthcare costs, but there is currently a limited number of studies evaluating direct medical costs in elderly people with co-existing diabetes and frailty.
Objective: To explore factors associated with total direct medical costs in elderly patients with diabetes and frailty.
Methods: A cross-sectional descriptive study was conducted on 166 outpatients at a rural health center in Vietnam. Supervised predictive models, including linear regression and selected machine learning methods, were applied to predict direct medical costs.
Results: Marital status, living with family, and duration of diabetes were the three variables with the highest level of importance in contributing to the predictive ability of the model. Unmarried and divorced individuals had lower costs compared to the married group (β = −0.29; 95% CI: −0.51 to −0.07; p = 0.009). Similarly, those living with family were associated with lower costs compared to those not living with family (β = −0.29; 95% CI: −0.50 to −0.08; p = 0.008). Duration of diabetes was positively associated with cost (β = 0.04; 95% CI: 0.00 to 0.09; p = 0.046).
Conclusions: Social and health-related factors are associated with total direct medical costs among frail older adults with diabetes mellitus. Healthcare managers and policymakers should consider these factors when planning, designing, and implementing healthcare policies for older adults.
Keywords: costs and cost analyses; diabetes mellitus; frailty; socioeconomic factors; Vietnam.
RESUMEN
Antecedentes: La diabetes mellitus y la fragilidad se asocian con un aumento de los costos sanitarios; sin embargo, existen pocos estudios que evalúen los costos médicos directos en personas mayores con diabetes y fragilidad concomitantes.
Objetivo: Explorar los factores asociados con costos médicos directos totals en pacientes adultos mayores con diabetes y fragilidad.
Métodos: Se realizó un estudio descriptivo transversal en 166 pacientes ambulatorios atendidos en un centro de salud rural de Vietnam. Se aplicaron modelos predictivos supervisados, incluida la regresión lineal y métodos seleccionados de aprendizaje automático, para predecir los costos médicos directos.
Resultados: El estado civil, convivir con la familia y la duración de la diabetes fueron las tres variables con mayor importancia para la capacidad predictiva del modelo. Las personas solteras o divorciadas tuvieron menores costos que las casadas (β = −0,29; IC95 %: −0,51 a −0,07; p = 0,009). Asimismo, quienes vivían con la familia se asociaron con menores costos que quienes no vivían con la familia (β = −0,29; IC95 %: −0,50 a −0,08; p = 0,008). La duración de la diabetes se asoció positivamente con el costo (β = 0,04; IC95 %: 0,00 a 0,09; p = 0.046).
Conclusiones: Los factores sociales y los relacionados con la salud se asocian con los costos médicos directos totales en adultos mayores frágiles con diabetes mellitus. Los gestores y responsables de políticas deberían considerar estos factores al planificar, diseñar e implementar políticas sanitarias para personas mayores.
Palabras clave: costos y análisis de costos; diabetes mellitus; factores socioeconómicos; fragilidad; Vietnam.
Received: 07/01/2026
Approved: 11/02/2026
INTRODUCTION
Diabetes mellitus and frailty are two conditions that often occur concurrently, tend to increase significantly with age, and are increasingly common in older adults.(1,2) The highest prevalence of diabetes mellitus is reported in those over 65 years of age, with an estimated 23.7% in the 65–99 age group.(3) In Vietnam, the number of people with diabetes is projected to increase from 5.2 million (6.8% of the adult population) in 2021 to 7.4 million by 2045, while only 28.9% of patients receive treatment at healthcare facilities.(4) Diabetes mellitus is associated with increasing frailty and functional decline in older adults and may explain up to 20% of the increased risk of disability in this age group.(5) In low- and middle-income countries, the prevalence of frailty is 17.4%.(6) Whether occurring individually or concurrently, diabetes mellitus and frailty have negative impacts on the psychosocial health of older adults, such as depression, reduced quality of life, and an increased risk of poor health outcomes, such as death.(7,8,9) These conditions simultaneously significantly increase the demand for healthcare services, leading to an increase in total healthcare costs.(1)
Globally, the annual cost per patient with diabetes ranges from US$87 to US$9,581.(10) In Vietnam, the annual cost per patient with diabetes ranges from VND 6,505,416 to VND 9,816,660, with inpatient treatment costs ranging from VND 2,076,737 to VND 3,694,295 and outpatient costs ranging from VND 462,588 to VND 2,836,387.(11) Frailty increases healthcare utilization among patients with type 2 diabetes.(12) Specifically, frailty significantly increases average total costs by US$4,653 compared to the costs of those in the robust group.(13) In a study of adults with type 2 diabetes and overweight or obesity, compared to the least frail group, those in the most frail group at year 1 had higher medication, outpatient, and hospitalization costs of US$714 (42% increase), US$244 (22% increase), and US$800 (134% increase), respectively.(14)
Factors associated with higher medical costs in elderly people with diabetes were found to include being female, living in rural communities, being dually eligible, having complications, and renal impairment,(15,16) due to an increased frequency of outpatient visits, as well as a higher likelihood of inpatient treatment and longer hospital stays.(17) Additionally, in frail individuals, factors such as weight loss, comorbidity, exhaustion, and limitations in basic and instrumental activities of daily living were found to be associated with higher healthcare costs.(18,19,20) However, there is currently a limited number of studies evaluating medical costs in elderly people with co-existing diabetes and frailty. Therefore, this study was conducted with the aim of exploring factors associated with total direct medical costs in elderly patients with diabetes and frailty.
METHODS
Study design
A cross-sectional descriptive study was conducted at the Outpatient and Interdisciplinary Department of a rural health center in Vietnam. The study analyzed the costs of eligible outpatient patients with diabetes and frailty from May 2025 to December 2025.
Study population
Inclusion criteria included: patients aged 60 years or older; diagnosed with diabetes or previously diagnosed with diabetes and currently taking diabetes medication; and diagnosed with frailty according to the FRAIL scale using the validated Vietnamese version by Do T et al.(21) Patients who were unable to answer the research questions or who did not consent to participate were excluded.
Data collection
Participants were selected using a convenience sampling method, which included all patients meeting the inclusion and exclusion criteria during the study period. The study was conducted among patients with diabetes and frailty who visited the outpatient department of the health center. While waiting for their turn, participants were introduced to the study objectives and content and invited to participate. Written consent was obtained before the study began. Participants were interviewed in person for approximately 10–15 minutes, and the interviewer completed a paper questionnaire.
Demographic and health-related characteristics of participants were collected, including gender (men and women), age (years), religion (non-Buddhist and Buddhist), education (primary, lower secondary, upper secondary, and tertiary), occupation (farmer, homemaker, retired, not working, and other), marital status (married, widowed, single, and divorced), living with family (yes and no), poverty status (yes and no), monthly income (million VND), diabetes-related complications (yes and no), duration of diabetes (years), number of medications (count), and fasting blood glucose level (mmol/L).
Data were collected through interviews and, where appropriate, extracted from patients’ electronic records. Costs assessed in this study were direct medical costs, including outpatient consultation, laboratory tests, diagnostic imaging and functional tests, medicines, and medical consumables, which were extracted from patients’ electronic records.
Statistical analysis
Data were entered and analyzed using IBM-SPSS version 22. Continuous variables were presented as the mean and standard deviation (SD), while categorical variables were presented as frequencies and percentages (%). Supervised predictive models, including linear regression, support vector machine (SVM), decision tree regression, and random forest, were used for prediction. Medical cost data were split into training and test sets at an 8:2 ratio. Model performance was evaluated using mean squared error (MSE), root mean square error (RMSE), mean absolute error (MAE), mean absolute percentage error (MAPE), and the coefficient of determination (R²). To assess feature importance, the study used a mean dropout loss–based method, with a larger mean dropout loss reflecting higher importance of the corresponding variable. Analyses of predictive models were performed using JASP 0.19.1. Multivariable regression analysis was used to identify factors associated with log-transformed total direct medical costs. A p-value of less than 0.05 was considered statistically significant.
Ethical considerations
This study was conducted in accordance with the Declaration of Helsinki. The study was approved by the Ethics Committee for Biomedical Research at Can Tho University of Medicine and Pharmacy (IRB No. 25.158.HV/PCT-HDDD).
RESULTS
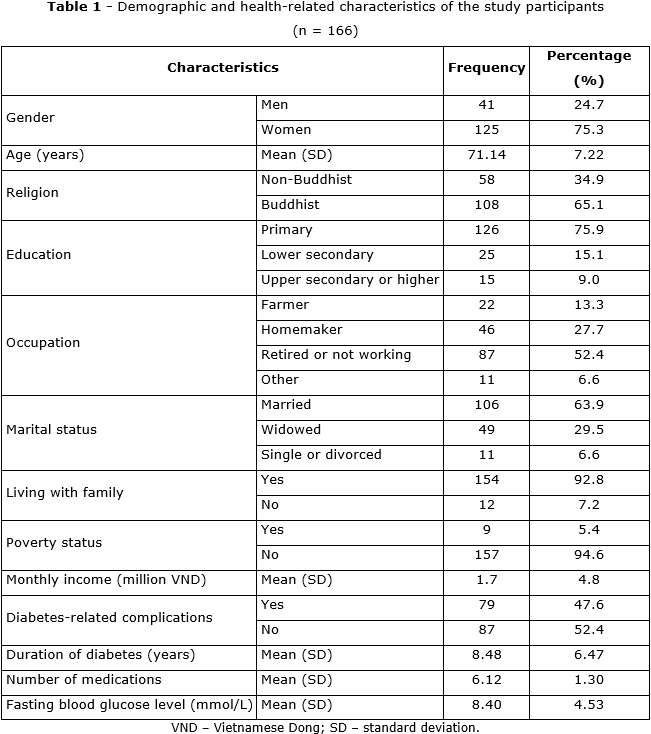
Individuals with diabetes and frailty (n = 166) participated in the study (table 1). The average age of participants was 71.14 years (SD = 7.22). The majority were women (75.3%), Buddhist (65.1%), married (63.9%), and had primary education (75.9%). More than half of the participants were retired or did not work (52.4%). A smaller proportion did not live with family (7.2%) and had poverty status (5.4%). Nearly half of the participants had diabetic complications (47.6%). The average duration of diabetes was 8.48 years (SD = 6.47) and the average fasting blood glucose was 8.40 (SD = 4.53).
Direct medical costs per outpatient treatment episode are presented in table 2. The total mean direct medical cost per outpatient treatment episode was 249,423 VND. Within the service categories, medicines accounted for the largest proportion, with a mean cost of VND 178,073, equivalent to 71.4% of total direct medical costs. When analyzed by payer, the majority of costs were covered by health insurance funds, with a mean cost of VND 244,057, accounting for 97.8% of total direct medical costs.
Performance evaluation of the four predictive models, presented in table 3, showed that linear regression provided the highest explained variance and the lowest error metrics with Test MSE = 0.040, RMSE = 0.200, MAE = 0.129 and MAPE = 5.24%, R² = 0.205. Therefore, linear regression has the potential to be more stable, and a more accurate predictor compared to the other models in the context of this study’s data. Figure 1 presents the relative importance of variables in the linear regression model, assessed based on mean dropout loss. The results showed that marital status, living with family, and duration of diabetes were the three variables with the highest level of importance in contributing to the predictive ability of the model.
The multivariable linear regression analysis found that the three variables, including marital status, living with family, and duration of diabetes, were statistically significantly associated with total direct medical costs (table 4). Unmarried and divorced individuals had lower costs compared to the married group (β = −0.29; 95% CI: −0.51 to −0.07; p = 0.009). Similarly, those living with family were associated with lower costs compared to those not living with family (β = −0.29; 95% CI: −0.50 to −0.08; p = 0.008). Conversely, duration of diabetes was positively associated with cost (β = 0.04; 95% CI: 0.00 to 0.09; p = 0.046).
DISCUSSION
The current study has demonstrated that marital status, living with family, and duration of diabetes were associated with total direct medical costs among frail older adults with diabetes mellitus. Analysis of the importance of the study variables and the results of the multivariable regression both show that several social and clinical factors such as marital status, living with family, and duration of diabetes contribute significantly to direct medical costs. The study results may provide useful information for healthcare planning and resource allocation, and our findings may highlight the potential use of machine learning and regression-based predictive methods in real-world clinical settings when conducting economic analyses to support decision-making.
Unmarried and divorced individuals had lower costs compared to the married group. Compared to the married group, the lower costs in the unmarried/divorced group may reflect a tendency towards lower outpatient use, as unmarried/divorced individuals are often less supported in their regular check-ups and monitoring than those with a partner; evidence suggests that the unmarried group tends to have fewer recent outpatient visits than married individuals.(22) Furthermore, the lower costs in this group may not be due to better health, but rather to greater mobility difficulties, less participation in preventive health services, fewer support resources (e.g., health insurance and disposable income), or psychological barriers such as depression, leading to missed access to necessary health services.(22,23,24,25)
Similarly, those living with family were associated with lower costs compared to those not living with family. Living with family members such as children, grandchildren, siblings, etc., not necessarily spouses, where relatives often act as gatekeepers in health decisions, can help improve diabetes self-management by encouraging compliance through reminders,(26) which may affect patterns of healthcare use and costs. Support from informal caregivers that helps better manage blood glucose levels at home can reduce the frequency of acute complications, thereby minimizing the need for additional diagnostic tests or expensive medications during outpatient visits. In the Vietnamese context, care for the elderly and chronically ill patients still relies primarily on family, so living with family can influence healthcare use and costs.(27)
In diabetic patients, frailty is associated with increased use of healthcare services. The development and progression of frailty in older adults with diabetes leads to adverse outcomes such as increased risk of falls, injuries, fractures, dementia, disability, poor quality of life, and death.(28) These consequences increase the need for healthcare services such as hospitalization and facility-based care, thereby increasing total direct medical costs.(28) In addition, direct medical costs tend to increase with the duration of the disease; on average, for diabetic patients alone, each year of the disease increases annual healthcare costs by an additional US$158.(29) Therefore, diabetic patients with comorbid conditions and longer disease duration are likely to face a higher burden of direct medical costs.
This study offers additional details about the limited knowledge of treatment costs among individuals with diabetes and frailty within the context of a rural health facility in Vietnam. However, this study has some limitations. First, this study was conducted at a single rural health center in Vietnam. Results may vary depending on the region, especially urban areas. Second, we only applied general-purpose predictive models implemented within a machine-learning framework. Some custom-designed models may offer better performance. Finally, demographic information and health status were limited. Additional data sources may need to be included, such as adherence levels, specific complication types, functional indicators, or socioeconomic determinants of health. Future work will address some of these limitations. In future studies, the authors plan to expand the analysis to multiple centers, including urban areas. Furthermore, our future research will involve clinicians and policy experts to make the models clinically meaningful by integrating expertise in this field, such as variable selection and model interpretation, to better guide preventive interventions.
Medicines accounted for the largest proportion of total direct medical costs among frail older adults with diabetes mellitus. Marital status, living with family, and duration of diabetes contribute significantly to direct medical costs. Healthcare managers and policymakers should consider these factors when planning, designing, and implementing healthcare policies for older adults.
BIBLIOGRAPHIC REFERENCES
1. Abd Ghafar MZA, O’Donovan M, Sezgin D, Moloney E, Rodríguez-Laso Á, Liew A, et al. Frailty and diabetes in older adults: Overview of current controversies and challenges in clinical practice [Internet]. Front Clin Diabetes Healthc. 2022;3:895313. DOI: https://www.doi.org/10.3389/fcdhc.2022.895313
2. Cobo A, Vázquez LA, Reviriego J, Rodríguez-Mañas L. Impact of frailty in older patients with diabetes mellitus: An overview [Internet]. Endocrinol Nutr. 2016;63(6):291–303. DOI: https://www.doi.org/10.1016/j.endonu.2016.01.004
3. Magliano D, Boyko E. Diabetes Atlas 11th edition scientific committee [Internet]. Brussels: International Diabetes Federation; 2025. DOI: https://diabetesatlas.org/
4. Le MH, Le ND, Le TTN, Nguyen MC, Tran V De. Psychosocial factors associated with medication burden among patients with type 2 diabetes mellitus: A Cross-Sectional Study [Internet]. J Diabetes Res. 2025;2025:8885209. DOI: https://www.doi.org/10.1155/jdr/8885209
5. Peña-Longobardo LM, Oliva-Moreno J, Zozaya N, Aranda-Reneo I, Trapero-Bertran M, Laosa O, et al. Economic evaluation of a multimodal intervention in pre-frail and frail older people with diabetes mellitus: the MID-FRAIL project [Internet]. Expert Rev Pharmacoecon Outcomes Res. 2021;21(1):111–8. DOI: https://www.doi.org/10.1080/14737167.2020.1766970
6. Siriwardhana DD, Hardoon S, Rait G, Weerasinghe MC, Walters KR. Prevalence of frailty and prefrailty among community-dwelling older adults in low-income and middle-income countries: a systematic review and meta-analysis [Internet]. BMJ Open. 2018;8(3):e018195. DOI: https://www.doi.org/10.1136/bmjopen-2017-018195
7. Duluklu B, Ivory J, McElvaney A, Bligh A, Cahill‐Collins M, Gethin G, et al. Frailty and comorbidity in older adults with and without diabetes and chronic leg ulcer: A cross‐sectional study [Internet]. Int Wound J. 2025;22(1): e70119. DOI: https://www.doi.org/10.1111/iwj.70119
8. O’Donovan M, Sezgin D, O’Caoimh R, Liew A. The relationship between frailty and diabetes: An investigation of self-rated health, depression symptoms and quality of life in the Study of Health Aging and Retirement in Europe [Internet]. Arch Gerontol Geriatr. 2021;96:104448. DOI: https://www.doi.org/10.1016/j.archger.2021.104448
9. Shi J, Tao Y, Wang L, Chen S, Zhou Z, Meng L, et al. Combined effect of diabetes and frailty on mortality among Chinese older adults: A follow-up study [Internet]. Front Endocrinol (Lausanne). 2023; 13:1105957. DOI: https://www.doi.org/10.3389/fendo.2022.1105957
10. Butt MD, Ong SC, Rafiq A, Kalam MN, Sajjad A, Abdullah M, et al. A systematic review of the economic burden of diabetes mellitus: contrasting perspectives from high and low middle-income countries [Internet]. J Pharm Policy Pract. 2024;17(1):2322107. DOI: https://www.doi.org/10.1080/20523211.2024.2322107
11. Ho TTH, Vo TH, Do QD, Chung KK, Nguyen LV, Vo NYN. A systematic review of treatment cost of type 2 diabetes in Vietnam [Internet]. Hong Bang Int Univ J Sci. 2023;24:39–46. DOI: https://www.doi.org/10.59294/HIUJS.24.2023.311
12. Chao C-T, Wang J, Chien K-L, COhort of GEriatric Nephrology in NTUH (COGENT) study group. Both pre-frailty and frailty increase healthcare utilization and adverse health outcomes in patients with type 2 diabetes mellitus [Internet]. Cardiovasc Diabetol. 2018;17(1):130. DOI: https://www.doi.org/10.1186/s12933-018-0772-2
13. Pradana AA, Bai D, Hidayat AT, Lin C-J, Lee S-C. Cost of illness analysis of frailty for older adults: a systematic review and meta-analysis [Internet]. Eur Geriatr Med. 2025;16(1):149–62. DOI: https://www.doi.org/10.1007/s41999-024-01123-6
14. Espeland MA, Harada ASM, Ross J, Bancks MP, Pajewski NM, Simpson FR, et al. Cross-sectional and longitudinal associations among healthcare costs and deficit accumulation [Internet]. J Am Geriatr Soc. 2024;72(9):2759–69. DOI: https://www.doi.org/10.1111/jgs.19053
15. Liaw W, Adepoju OE, Luo J, Glasheen B, King B, Kakadiaris I, et al. Factors Associated with Health Care Costs in Older Adults with Type 2 Diabetes: Insights for Value-Based Payment Models [Internet]. Popul Health Manag. 2025;28(4):191–7. DOI: https://www.doi.org/10.1089/pop.2025.0054
16. Guerrero-Fernández de Alba I, Orlando V, Monetti VM, Mucherino S, Gimeno-Miguel A, Vaccaro O, et al. Comorbidity in an Older Population with Type-2 Diabetes Mellitus: Identification of the Characteristics and Healthcare Utilization of High-Cost Patients [Internet]. Front Pharmacol. 2020; 11:586187. DOI: https://www.doi.org/10.3389/fphar.2020.586187
17. Nari F, Park E-C, Nam C-M, Jang S-I. Impact of frailty on mortality and healthcare costs and utilization among older adults in South Korea [Internet]. Sci Rep. 2023;13(1):21203. DOI: https://www.doi.org/10.1038/s41598-023-48403-y
18. Hajek A, Bock JO, Saum KU, Matschinger H, Brenner H, Holleczek B, et al. Frailty and healthcare costs—longitudinal results of a prospective cohort study [Internet]. Age Ageing. 2018;47(2):233–41. DOI: https://www.doi.org/10.1093/ageing/afx157
19. García-Nogueras I, Aranda-Reneo I, Peña-Longobardo LM, Oliva-Moreno J, Abizanda P. Use of health resources and healthcare costs associated with frailty: The FRADEA study [Internet]. J Nutr Health Aging. 2017;21(2):207–14. DOI: https://www.doi.org/10.1007/s12603-016-0727-9
20. Bock JO, König HH, Brenner H, Haefeli WE, Quinzler R, Matschinger H, et al. Associations of frailty with health care costs – results of the ESTHER cohort study [Internet]. BMC Health Serv Res. 2016;16(1):128. DOI: https://www.doi.org/10.1186/s12913-016-1360-3
21. Do TNA, Nguyen TTT, Nguyen TC, Nguyen T Van. The Validity of The FRAIL Scale in Frailty Screening Among Vietnamese Older People [Internet]. Aging Med Healthc. 2022;13(2):87–92. DOI: https://www.doi.org/10.33879/AMH.132.2021.07060
22. Pandey KR, Yang F, Cagney KA, Smieliauskas F, Meltzer DO, Ruhnke GW. The impact of marital status on health care utilization among Medicare beneficiaries [Internet]. Medicine. 2019;98(12):e14871. DOI: https://www.doi.org/10.1097/MD.0000000000014871
23. Hossain B, Yadav PK, Nagargoje VP, Vinod Joseph KJ. Association between physical limitations and depressive symptoms among Indian elderly: marital status as a moderator [Internet]. BMC Psychiatry. 2021;21(1):573. DOI: https://www.doi.org/10.1186/s12888-021-03587-3
24. Hossain B, Yadav PK, Nagargoje VP, Vinod Joseph KJ. Association between physical limitations and depressive symptoms among Indian elderly: marital status as a moderator [Internet]. BMC Psychiatry. 2021;21(1):573. DOI: https://www.doi.org/10.1186/s12888-021-03587-3
25. Stafford M, von Wagner C, Perman S, Taylor J, Kuh D, Sheringham J. Social connectedness and engagement in preventive health services: an analysis of data from a prospective cohort study [Internet]. Lancet Public Health. 2018;3(9):e438–46. DOI: https://www.doi.org/10.1016/S2468-2667(18)30141-5
26. Alodhailah AM, Lam L, Almutairi AA, Alahmedi SH, Alsadoun A, Almutairi M, et al. Exploring healthcare professionals’ perspectives on barriers and enablers of antiplatelet adherence after PCI: a multisite qualitative study in Saudi Arabia [Internet]. BMC Nurs. 2025;24(1):1393. DOI: https://www.doi.org/10.1186/s12912-025-04067-9
27. Viet Nam Social Security. Workshop discusses elderly care in Vietnam [Internet]. Viet Nam Social Security; 2026. DOI: https://vss.gov.vn/english/news/Pages/vietnam-social-security.aspx?CateID=0&ItemID=10444
28. Abdelhafiz D, Abdelhafiz A. Practical Considerations in the Management of Frail Older People with Diabetes [Internet]. Diseases. 2025;13(8):249. DOI: https://www.doi.org/10.3390/diseases13080249
29. Trogdon JG, Hylands T. Nationally representative medical costs of diabetes by time since diagnosis [Internet]. Diabetes Care. 2008;31(12):2307–11. DOI: https://www.doi.org/10.2337/dc08-1375
Acknowledgements
We acknowledge the Can Tho University of Medicine and Pharmacy and outpatients for their collaboration in this study.
Conflict of interests
The authors have no conflicts of interest to declare.
Financial information
There was no external funding for this research.
Authorship contribution
Conceptualization: Ngoc Tuyet Nguyen, Quoc Cuong Hoang, Van De Tran.
Data curation: Ngoc Tuyet Nguyen.
Formal analysis: Ngoc Tuyet Nguyen, Minh Trung Nguyen, Van De Tran.
Investigation: Ngoc Tuyet Nguyen, Van De Tran.
Methodology: Ngoc Tuyet Nguyen, Quoc Cuong Hoang, Van De Tran.
Supervision: Quoc Cuong Hoang, Van De Tran.
Writing – original draft: Ngoc Tuyet Nguyen, Quoc Cuong Hoang, Minh Trung Nguyen, Van De Tran.
Writing – review & editing: Ngoc Tuyet Nguyen, Quoc Cuong Hoang, Minh Trung Nguyen, Van De Tran.
Data availability
The data that support the findings of this study are available from the corresponding authors (i.e., upon reasonable request).