Research Article
The economic impact of potentially inappropriate medications in older stroke patients: a comparison of criteria
Impacto económico de los medicamentos potencialmente inapropiados en pacientes adultos mayores con ictus: comparación de criterios
Tho Kieu Anh Pham1 https://orcid.org/0000-0002-0917-1805
Thi Bui Nhu Ngoc Ho1 https://orcid.org/0009-0006-3196-0559
Rebecca Susan Dewey2 https://orcid.org/0000-0002-6888-3298
Van De Tran1* https://orcid.org/0000-0003-0421-5079
1Can Tho University of Medicine and Pharmacy. Can Tho, Vietnam.
2University of Nottingham. Nottingham, United Kingdom.
*Corresponding author. Email: tvde@ctump.edu.vn
ABSTRACT
Background: Potentially inappropriate medications (PIMs) disproportionally affect the quality of life of patients aged 65 years or older and are associated with increased direct healthcare costs. However, evidence on their economic impact remains limited in the Vietnamese context.
Objectives: To compare the potential costs associated with PIMs as measured using three tools (Beers, STOPP/START, and MALPIP), in elderly stroke patients.
Methods: A descriptive cross-sectional study was conducted in 300 acute stroke patients aged 65 years and older receiving inpatient treatment at a hospital in Can Tho City, Vietnam, from January to July 2024.
Results: The mean total direct healthcare cost per patient was VND 2,918,149. STOPP/START produced the highest estimated savings across all scenarios. Under the 100% discontinuation scenario, the total cost savings were VND 117,637 per patient per treatment episode, including VND 109,416 saved by the health insurance fund and VND 8,221 saved in patient out-of-pocket payments.
Conclusion: The STOPP/START tool may better identify potentially avoidable medication-related costs. Healthcare professionals should consider integrating STOPP/START into routine medication reviews to help reduce unnecessary medication costs among older patients with stroke.
Keywords: cost savings; potentially inappropriate medication list; stroke; Vietnam.
RESUMEN
Antecedentes: Los medicamentos potencialmente inapropiados (PIMs) afectan de manera desproporcionada la calidad de vida de los pacientes de 65 años o más y se asocian con un aumento de los costos directos de atención sanitaria. Sin embargo, la evidencia sobre su impacto económico sigue siendo limitada en el contexto vietnamita.
Objetivos: Comparar los costos potenciales asociados con los PIMs medidos mediante tres herramientas (Beers, STOPP/START y MALPIP) en pacientes adultos mayores con accidente cerebrovascular.
Métodos: Se realizó un estudio transversal descriptivo en 300 pacientes con accidente cerebrovascular agudo de 65 años o más, que recibían tratamiento hospitalario en un centro de la ciudad de Can Tho, Vietnam, entre enero y julio de 2024.
Resultados: El costo promedio total directo de atención sanitaria por paciente fue de 2.918.149 VND. La herramienta STOPP/START generó los mayores ahorros estimados en todos los escenarios. Bajo el escenario de suspensión del 100 %, el ahorro total de costos fue de 117.637 VND por paciente por episodio de tratamiento, incluyendo 109.416 VND ahorrados por el fondo de seguro de salud y 8.221 VND ahorrados en gastos de bolsillo de los pacientes.
Conclusión: La herramienta STOPP/START puede identificar mejor los costos potencialmente evitables relacionados con los medicamentos. Los profesionales de la salud deberían considerar integrar STOPP/START en las revisiones rutinarias de la medicación para ayudar a reducir los costos innecesarios de medicamentos en pacientes mayores con accidente cerebrovascular.
Palabras clave: accidente cerebrovascular; ahorro de costos; medicamentos potencialmente inapropriados; Vietnam.
Received: 07/03/2026
Approved: 16/04/2026
INTRODUCTION
The rapid aging of the global population poses significant challenges to healthcare systems,(1) pension and insurance systems, social assistance models, and socio-economic growth.(2) One of the major health problems among older adults worldwide is stroke.(3) Stroke is a leading cause of disability and death and imposes a substantial economic burden due to the costs of acute treatment and post-stroke care.(4) The estimated global prevalence of stroke among older adults is 7.4%.(5) In low- and middle-income countries such as Vietnam, stroke mortality rates are increasing in parallel with the growing burden of chronic diseases,(6) with the most vulnerable groups being adults aged 60–64 and 65–69 years.(7) The age-standardized stroke incidence rate in Vietnam is 203.36 per 100,000 population, exceeding 187.98 in Southeast Asia and 141.55 globally.(8)
Older patients often have multiple chronic conditions, and the use of multiple medications is common and often unavoidable.(9) Multiple medication use is also common after stroke for secondary prevention and management of comorbidities.(10) In patients with stroke, polypharmacy is associated with poorer functional outcomes, a lower likelihood of discharge home, greater severity of post-stroke fatigue, progression of cognitive impairment, and an increased risk of falls.(11) Polypharmacy also increases the risk of potentially inappropriate medication (PIM) use (10) PIM use is common, with prevalence ranging from 11.6% to 43.6% in Asian countries.(12) A previous study in older adults with ischemic stroke reported that 43.29% of patients used at least one PIM.(13) In Vietnam, the prevalence of potentially inappropriate medications use among hospitalized older patients is 31.2%.(14)
Potentially inappropriate medications (PIMs) can be defined as medications for which the potential risks (e.g., adverse drug events) outweigh the potential benefits in older adults, particularly when safer or more effective alternatives exist.(15) PIMs are a major health concern affecting the quality of life of patients aged 65 years and older and are associated with adverse drug events (including falls), increased healthcare costs, greater healthcare use, and hospitalization.(16) To address this issue, several screening tools have been developed to identify and reduce PIM use, such as the Beers Criteria,(17) the STOPP/START criteria,(18) and the MALPIP tool.(19) Using these tools, many studies worldwide have examined the cost impact of PIMs.(20,21,22,23) However, evidence in Vietnam remains limited. Therefore, this study aims to compare the performance of the Beers, STOPP/START, and MALPIP tools in estimating the cost impact of PIMs among older patients with stroke in a hospital in Vietnam.
METHODS
Study design
This study used a descriptive cross-sectional design in older patients hospitalized with acute stroke at a first-class hospital in Can Tho City, Vietnam, from January 1, 2024 to July 30, 2024. Can Tho City has a population of approximately 1.3 million people.(24)
Eligible participants were aged 65 years or older, had a diagnosis of stroke (ischemic or hemorrhagic) based on ICD-10, and received inpatient treatment at the study hospital. Exclusion criteria were incomplete medical records; death or transfer within 24 hours of admission; and patients treated exclusively with traditional medicine.
Sample size
The sample size was calculated using the single-proportion formula, assuming a 95% confidence level, a margin of error of 4%, and an estimated PIM prevalence of 89.1% based on MALPIP from previous research.(20) The minimum required sample size was 234 patients.
Data collection and variables
Patient data were collected from medical records in the hospital's paper archive. Demographic and health-related information collected included age, sex, comorbidities, and length of hospital stay. Information on direct medical costs was also collected, such as medications, tests, medical supplies, imaging, functional tests, procedures, and surgery. Data collection was performed by trained data collectors, and data entry was also performed by another data collector in parallel to ensure data entry accuracy.
The Beers, STOPP/START and MALPIP tools were used to identify potentially inappropriate medications (PIMs).(14,17,18,19,25) For each patient, all medications used during inpatient treatment were evaluated for PIMs using these tools, and then categorized by type and frequency.
In this study, three intervention scenarios were considered, as follows. Scenario A: discontinue all identified PIM-containing drugs; Scenario B: discontinue 50% of PIM-containing drugs; and Scenario C: discontinue only 25% of PIM-containing drugs. Based on the proposed scenarios, the total cost savings for each tool (Beers 2023, STOPP/START version 3, and MALPIP 2022) were calculated.
Statistical analysis
Data were analyzed using SPSS Statistics version 26.0. Descriptive categorical variables such as frequency (n) and percentage (%) were used; while continuous variables used were mean and standard deviation (SD). The Cohen's Kappa coefficient (κ) was used to determine the agreement between the PIM screening tools. Indicators included total savings per patient per treatment cycle, average savings for the health insurance fund, and average savings for patient out-of-pocket payments.
Ethical considerations
The study was approved by the Ethics Review Board of Can Tho University of Medicine and Pharmacy (No. 25.040.HV.UD/PCT-HĐĐĐ).
RESULTS
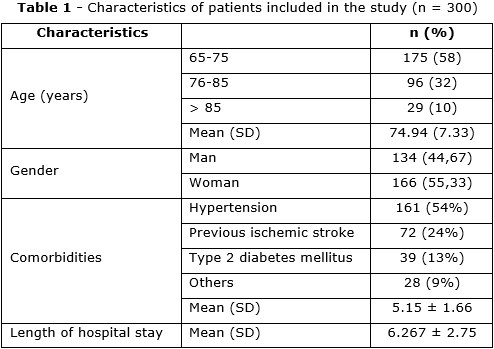
A total of 300 medical records of older patients hospitalized with acute stroke were included in the analysis. The mean age of participants was 74.94 years (SD = 7.33), with most patients aged 65–75 years (58%). Female patients accounted for a higher proportion than male patients (55.3% vs. 44.7%). On average, each patient had 5.15 comorbidities (SD = 1.66), with hypertension being the most common (54%). The mean length of hospital stay was 6.27 days (SD = 2.75) (table 1).
Agreement between the screening criteria was moderate between the Beers Criteria and MALPIP (κ = 0.449). In contrast, agreement between the Beers Criteria and STOPP/START (κ = 0.240) and between STOPP/START and MALPIP (κ = 0.216) was weak. MALPIP (2022) identified the highest proportion of patients with at least one PIM (189/300, 63%), followed by the 2023 Beers Criteria (99/300, 33%) and STOPP/START version 3 (84/300, 28%). The mean number of PIMs per patient with at least one PIM ranged from 2.35 to 2.93 across the three criteria. Common PIM categories differed by criteria, including loop diuretics and tricyclic antidepressants (Beers), fluoroquinolone antibiotics (STOPP/START), and psychotropic drugs and NSAIDs (MALPIP) (table 2).
The total direct medical cost was VND 875,444,822 (USD 36,227), with a mean of VND 2,918,149 per patient (SD = VND 1,585,568) (table 3). Diagnostic imaging accounted for the largest share (65%; VND 570,949,800), followed by medications (17%; VND 150,786,190) and laboratory tests (13%; VND 109,653,500). The remaining components accounted for a small proportion of the total (1–2%).
STOPP/START was associated with the highest estimated cost savings across all scenarios. Under the 100% discontinuation scenario, the total cost savings were VND 117,637 per patient per treatment episode, of which the mean savings for the health insurance fund were VND 109,416 per patient per treatment episode (table 4).
DISCUSSION
This study was conducted using the hospital records of 300 older stroke patients at a first-class hospital in Can Tho City, a particularly vulnerable population due to the high burden of comorbidities (mean 5.15 ± 1.66 conditions). Multimorbidity is commonly accompanied by polypharmacy, thereby increasing the risk of PIMs. The prevalence of PIMs in this study varied substantially depending on the screening tool used: MALPIP 2022 identified PIMs in 63% of medical records, the 2023 Beers Criteria in 33%, and STOPP/START version 3 in 28%. The prevalence of PIMs according to the Beers Criteria (33%) is comparable with findings from previous studies in Vietnam, such as that by Le TH et al., which reported a rate of 31.2% among hospitalized older patients.(26) However, this rate is lower than that reported by a study in Ho Chi Minh City which recorded 41.5% according to Beers 2019 criteria in inpatients. This study found that PIMs had the highest rate (63%) in the MALPIP tool, which is similar to the findings of Chang CT et al.(20) in Malaysia, where a significantly higher rate of PIMs (89.1%) was recorded by the MALPIP tool. Although differences in context, population, and health system characteristics may affect these findings, it can be seen that MALPIP tends to detect higher rates of PIMs.
This research results found that the average direct medical cost for an inpatient treatment in elderly stroke patients was 2,918,149 VND. This result is lower than another study in Vietnam by Nguyen TV et al.,(27) which found the average direct medical cost per patient was 10.5 ± 7.3 million VND. This could be due to differences in drug prices, supplies, technical service prices, etc., at each medical facility, and also due to factors such as patients having different circumstances, stages, and levels of disease.(28) The present findings add to the data on the cost burden in the elderly patient group, which can provide policymakers with a more comprehensive view of the situation.
In the three scenarios applied, the STOPP/START criteria showed the highest potential for cost savings, although the rate of PIMs detected based on these criteria was the lowest. This result can be explained by the fact that the PIMs recorded based on the STOPP/START criteria were mainly drugs with higher prescription frequency and higher cost; while the PIMs recorded based on the Beers criteria were predominantly drugs with lower cost. These results differ from the findings of Chang CT et al. in Malaysia, where the MALPIP criteria were found to have the highest potential for economic efficiency.(20) This difference may stem from differences in drug prices and treatment guidelines in each country. In general, no single tool has been found that can optimize both the detection of PIMs and the cost of drugs used. Therefore, healthcare facilities should adopt a multi-tool strategy.
Limitations: This study has several limitations. Firstly, it was conducted at only one hospital in Can Tho, which may affect the generalizability of the findings. Future research should evaluate the cost-effectiveness of interventions that reduce the incidence of prescriptions related to PIMs to provide further evidence of clinical and economic benefits in clinical practice across healthcare settings. Additionally, future studies should be conducted across a wider range of healthcare settings to provide more generalizable evidence.
The STOPP/START tool has the greatest potential for cost savings related to potentially inappropriate medications. Integrating this tool into healthcare settings is essential to optimize medication costs for patients. Furthermore, cost-effectiveness assessments of dosage reduction measures are necessary in future research to provide more evidence of the benefits of dosage reduction in the elderly across different healthcare settings.
BIBLIOGRAPHIC REFERENCES
1. Kallestrup-Lamb M, Marin AOK, Menon S, Søgaard J. Aging populations and expenditures on health [Internet]. J Econ Ageing. 2024;29:100518. DOI: https://www.doi.org/10.1016/j.jeoa.2024.100518
2. Thanh Trong N, Thi Dong N, Thi Ly P. Population aging and economic growth: evidence from ASEAN countries [Internet]. Cogent Bus Manag. 2024;11(1): 2298055. DOI: https://www.doi.org/10.1080/23311975.2023.2298055
3. Dee M, Lennon O, O’Sullivan C. A systematic review of physical rehabilitation interventions for stroke in low and lower-middle income countries [Internet]. Disabil Rehabil. 2020;42(4):473–501. DOI: https://www.doi.org/10.1080/09638288.2018.1501617
4. Meng X, Wang A, Wang R, Xu Q, Wu S, Han Y. EE208 Direct cost and indirect cost of ischemic stroke in China [Internet]. Value Health. 2022;25(12):S93–S94. DOI: https://www.doi.org/10.1016/j.jval.2022.09.457
5. Rajati F, Rajati M, Rasulehvandi R, Kazeminia M. Prevalence of stroke in the elderly: A systematic review and meta-analysis [Internet]. Interdiscip Neurosurg. 2023;32:101746. DOI: https://www.doi.org/10.1016/j.inat.2023.101746
6. Ngoc NH, Thong NV, Hien LX, An NQ, Thuan ND. Predictors of ischemic stroke in elderly patients in Vietnam [Internet]. Genet Mol Res. 2021;20(1):1-12. DOI: https://www.doi.org/10.4238/gmr18741
7. Tran MC, Prisco L, Pham PM, Phan HQ, Ganau M, Pham N, et al. Comprehensive analysis of stroke epidemiology in Vietnam: Insights from GBD 1990–2019 and RES-Q 2017–2023 [Internet]. Glob Epidemiol. 2025;9:100199. DOI: https://www.doi.org/10.1016/j.gloepi.2025.100199
8. Truyen TTTT, Vo NLY, Vo QP, Phan TC, Le PNB, Nguyen HT, et al. Burden and risk factors of stroke in Vietnam from 1990 to 2021 – a systematic analysis from Global Burden of Disease 2021 [Internet]. J Stroke Cerebrovasc Dis. 2025;34(3):108241. DOI: https://www.doi.org/10.1016/j.jstrokecerebrovasdis.2025.108241
9. Tian X, Yu M, Sun Y, Yan H, Ma H, Jiang L, et al. Evidence-based summary for the safety of multiple medication in elderly patients with ischemic stroke [Internet]. Ann Transl Med. 2022;10(4):202. DOI: https://www.doi.org/10.21037/atm-22-453
10. Cadel L, Cimino SR, Bradley-Ridout G, Hitzig SL, Patel T, Ho CH, et al. Medication self-management interventions for persons with stroke: A scoping review [Internet]. PLoS One. 2023;18(5):e0285483. DOI: https://www.doi.org/10.1371/journal.pone.0285483
11. Barow E, Probst AC, Pinnschmidt H, Heinze M, Jensen M, Rimmele DL, et al. Effect of comorbidity burden and polypharmacy on poor functional outcome in acute ischemic stroke [Internet]. Clin Neuroradiol. 2023;33(1):147–154. DOI: https://www.doi.org/10.1007/s00062-022-01193-8
12. Lin YJ, Peng LN, Chen LK, Lin MH, Hwang SJ. Risk factors of potentially inappropriate medications among older patients visiting the community health center in rural Taiwan [Internet]. Arch Gerontol Geriatr. 2011;53(2):225–228. DOI: https://www.doi.org/10.1016/j.archger.2010.11.017
13. Tan X, Lv X, Xiong W, Liu Y, Zhang N. Prevalence and factors associated with potentially inappropriate medications in elderly stroke patients: A comparison of Beers 2019 and 2023 criteria [Internet]. Saudi Pharm J. 2025;33(4):27. DOI: https://www.doi.org/10.1007/s44446-025-00029-z
14. Nguyen VT, Bang AV, Dang TTP. Prevalence of potentially inappropriate medication use among hospitalized elderly patients and associated factors [Internet]. Vietnam J Community Med. 2023;64(3):1-7. DOI: https://www.doi.org/10.52163/yhc.v64i3.633
15. Cojuc-Konigsberg G, Schoo C. Inappropriate medication in the geriatric population [Internet]. Treasure Island: StatPearls Publishing; 2025 [access: 02/02/2026]. Available at: https://www.ncbi.nlm.nih.gov/books/NBK585118/
16. Alshammari H, Al-Saeed E, Ahmed Z, Aslanpour Z. Reviewing potentially inappropriate medication in hospitalized patients over 65 using explicit criteria: A systematic literature review [Internet]. Drug Healthc Patient Saf. 2021;13:183–210. DOI: https://www.doi.org/10.2147/DHPS.S303101
17. American Geriatrics Society. 2023 updated AGS Beers Criteria® for potentially inappropriate medication use in older adults [Internet]. J Am Geriatr Soc. 2023;71(7):2052–2081. DOI: https://www.doi.org/10.1111/jgs.18372
18. O’Mahony D, Cherubini A, Guiteras AR, Denkinger M, Beuscart JB, Onder G, et al. STOPP/START criteria for potentially inappropriate prescribing in older people: Version 3 [Internet]. Eur Geriatr Med. 2023;14(4):625–632. DOI: https://www.doi.org/10.1007/s41999-023-00777-y
19. Chang CT, Chan HK, Cheah WK, Tan MP, Ch'ng ASH, Thiam CN, et al. Development of a Malaysian potentially inappropriate prescribing screening tool in older adults (MALPIP): A Delphi study [Internet]. J Pharm Policy Pract. 2023;16(1):122. DOI: https://www.doi.org/10.1186/s40545-023-00630-4
20. Chang CT, Chan HK, Tan AY, Kamis SF, Yeo YL, Azman MA, et al. Comparing Beers, STOPP and MALPIP criteria in detecting potentially inappropriate medications, clinical outcomes, and cost impacts among older Malaysians: A cohort study [Internet]. J Pharm Policy Pract. 2024;17(1):2436896. DOI: https://www.doi.org/10.1080/20523211.2024.2436896
21. Heider D, Matschinger H, Meid AD, Quinzler R, Adler JB, Günster C, et al. The impact of potentially inappropriate medication on the development of health care costs and its moderation by the number of prescribed substances: Results of a retrospective matched cohort study [Internet]. PLoS One. 2018;13(7):e0198004. DOI: https://www.doi.org/10.1371/journal.pone.0198004
22. D’Aiuto C, Lunghi C, Guénette L, Berbiche D, Bertrand K, Vasiliadis HM. Health care system costs related to potentially inappropriate medication use involving opioids in older adults in Canada [Internet]. BMC Health Serv Res. 2023;23(1):1295. DOI: https://www.doi.org/10.1186/s12913-023-10303-2
23. Clark CM, Shaver AL, Aurelio LA, Feuerstein S, Wahler RG Jr, Daly CJ, et al. Potentially inappropriate medications are associated with increased healthcare utilization and costs [Internet]. J Am Geriatr Soc. 2020;68(11):2542–2550. DOI: https://www.doi.org/10.1111/jgs.16743
24. Tran HD, Hung TT, Thuy PTH, Tam LT, Tran HG, Le PH. Clinical features and treatment outcomes of COVID-19 admissions in the Can Tho City Hospital of Tuberculosis and Respiratory Diseases, Vietnam: A hospital-based observational study [Internet]. Healthcare (Basel). 2023;11(11): 1632. DOI: https://www.doi.org/10.3390/healthcare11111632
25. Thi NN, Thi KHH, Thi ATT, Ngoc HN, Huu TN. Analyzing inappropriate prescribing in the elderly by using Beers and STOPP/START criteria through clinical pharmaceutical activities at Nghi Loc General Hospital [Internet]. Vietnam Med J. 2022;515(2):117–122. DOI: https://www.doi.org/10.51298/vmj.v515i2.2770
26. Le TH, Nguyen NH. Evaluation of drug prescribing in the elderly inpatients using Beers criteria updated in 2019 [Internet]. Ho Chi Minh City J Med. 2020 [access: 02/02/2026];24(2):122–130. Available at: https://www.tapchiyhoctphcm.vn/articles/18141
27. Nguyen TV, Hoang MV, Doan HT, Nguyen VM. Direct medical cost for acute ischemic stroke patients in Vietnam [Internet]. J Popul Soc Stud. 2024;32:781–93. DOI: https://www.doi.org/10.25133/JPSSv322024.045
28. Than TTN, Nguyen TK, Nguyen VT. Study on direct medical costs in the treatment of acute ischemic stroke with alteplase at Binh Duong Provincial General Hospital in 2024–2025 [Internet]. Can Tho Med Pharm J. 2025;(88):246–52. DOI: https://www.doi.org/10.58490/ctump.2025i88.3567
Acknowledgements
We acknowledge the Can Tho University of Medicine and Pharmacy and patients for their collaboration in this study.
Conflict of interests
The authors have no conflicts of interest to declare.
Financial information
There was no external funding for this research.
Authorship contribution
Conceptualization: Tho Kieu Anh Pham, Thi Bui Nhu Ngoc Ho, Van De Tran.
Methodology: Tho Kieu Anh Pham, Thi Bui Nhu Ngoc Ho, Van De Tran.
Investigation: Tho Kieu Anh Pham, Thi Bui Nhu Ngoc Ho, Van De Tran.
Resources: Tho Kieu Anh Pham, Thi Bui Nhu Ngoc Ho, Rebecca Susan Dewey, Van De Tran.
Writing – original draft: Tho Kieu Anh Pham, Thi Bui Nhu Ngoc Ho, Rebecca Susan Dewey, Van De Tran.
Writing – review & editing: Tho Kieu Anh Pham, Thi Bui Nhu Ngoc Ho, Rebecca Susan Dewey, Van De Tran.
Data availability
The data that support the findings of this study are available from the corresponding authors (i.e., upon reasonable request).